
Case 34
Case 34 Content When this 78-year-old man walked into the clinic, he looked weary and depleted. For the past two days, he had been battling an intermittent fever topping 37.8°C, accompanied by a vanis
A 57-year-old woman with a long-standing history of bronchial asthma and COPD was admitted because of intermittent episodes of dyspnea associated with palpitations and general weakness for five days. At Emergency Department, she was afebrile but in moderate respiratory distress. BP measured 104/59 mmHg, PR 103/min, and RR 19/min. Physical findings were in line with COPD. There was jugular venous distension with an estimated JVP of 10 cm H2O. ECG showed sinus tachycardia at 103/min, diffuse low QRS voltage with right axis deviation (+120°), tall P wave in II, III, and aVF, and symmetrical T wave inversion involving V1-V5, suggesting RV strain/ischemia. Chest X-ray revealed a prominent pulmonary artery (bilateral) consistent with pulmonary hypertension. Specific laboratory tests under the suspicion of recurrent pulmonary embolism were ordered. ABG showed O2 Sat 97.0 %, pH 7.481 (N 7.35-7.45), pO2 80.6 (N 75-100) mmHg, pCO2 28.0 (N 32-45) mmHg, HCO3 20.4 (N 20-26) mmol/L, and BE -1.6 (N -2.0 – +2.0) mmol/L); BNP and D-dimer were 584 [N 100] pg/mL and 3770 [N 500] ng/mL, respectively. Complete blood count, BUN, Cr, bilirubin, PT, and aPTT were within normal limits, but GOT (56 [N5-40] IU/L and GPT (507 [N 7-56] IU/L) were elevated. Echocardiography revealed RV and RA enlargement with pulmonary hypertension (PH) (RVSP 90-105 mm Hg) and moderate-to-severe TR. Subsequent Chest CT demonstrated intraluminal filling defects in bilateral pulmonary arteries, confirming the diagnosis of pulmonary embolism. She immediately received IV heparin and oral warfarin in preparation for long-term anticoagulant therapy.
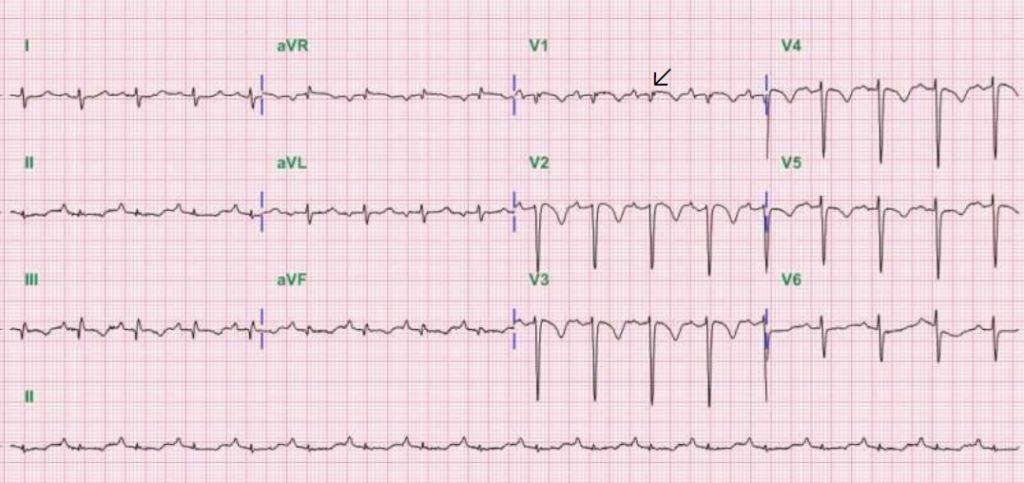
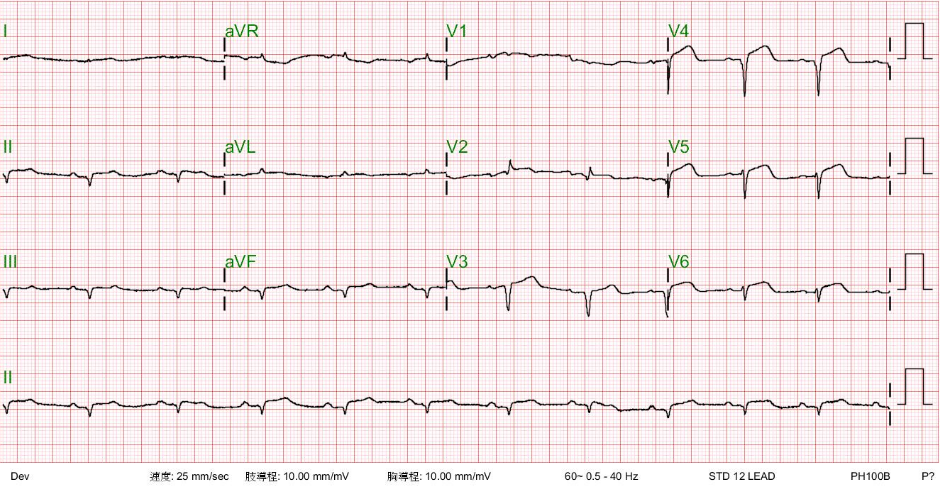
Sinus tachycardia at 103/min
Diffuse low QRS voltage with right axis deviation (+120°) and S1Q3 pattern.
Relatively tall P wave in II, III, and aVF (P pulmonale with COPD)
Propensity to RBBB in V1 (a subtle finding denoted by an arrow).
Symmetrical T wave inversion involving V1-V5.
The slow progression of the R wave in precordial leads (clockwise rotation of the heart)

Hyper-inflated lungs with prominent PA (bilateral) suggestive of pulmonary hypertension associated with COPD
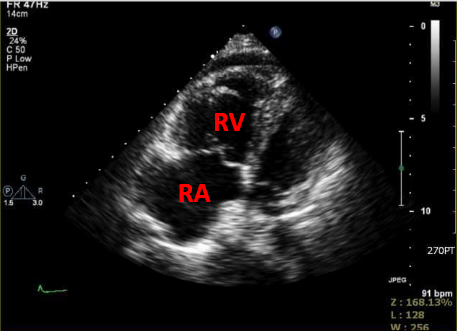
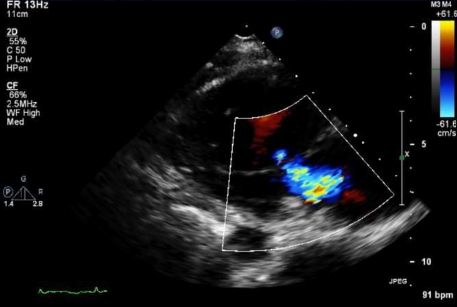
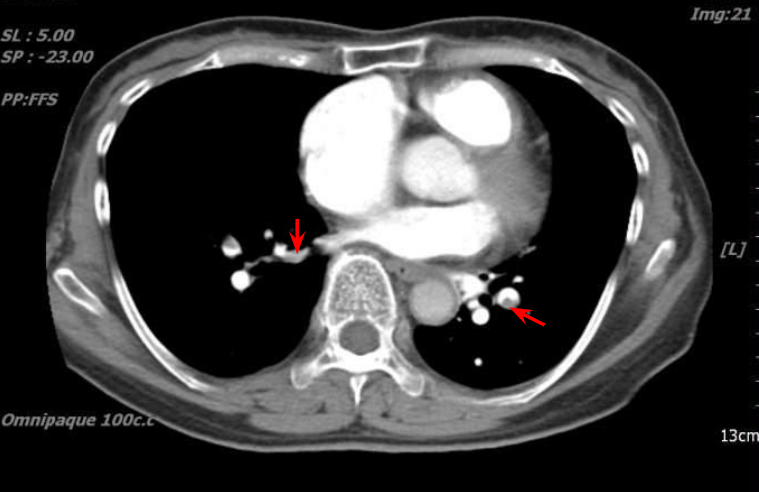
Intraluminal filling defects in bilateral pulmonary arteries.
Among all causes of respiratory deterioration, diagnosing pulmonary embolism in the presence of COPD is a clinical challenge. Dyspnea is the most frequent symptom of pulmonary embolism, whereas sinus tachycardia, albeit nonspecific, is the most common ECG finding.
The relatively tall P (P pulmonale) in the presence of diffuse low QRS voltage,* right axis deviation, and poor progression of R waves in precordial leads (clockwise rotation)** suggest that COPD is complicated by chronic pulmonary hypertension (PH). Prominent PA (bilateral) on chest X-ray and elevated JVP on physical examination provide further evidence supporting PH. Additionally, the propensity to RBBB in V1, the S1Q3 pattern, and symmetrical T inversion in V1-V5 *** further indicate RV strain/ischemia and are consistent with RV heart failure or acute pulmonary embolism. Echocardiography confirms RV and RA enlargement with PH (RVSP 90-105 mm Hg) and TR. Generally, a PH reading of 50 mmHg or more indicates its chronic nature, such as in long-standing COPD with or without pulmonary embolism.
The ABG findings (O2 Sat 97.0 %, pH 7.481, pO2 80.6 mmHg, pCO2 28.0 mmHg, HCO3 20.4 mmol/L, and BE -1.6 (N -2.0 – +2.0) mmol/L) indicate respiratory alkalosis with compensatory metabolic acidosis due to hypoxia and hyperventilation (hypocapnia), frequently observed during the early stage of pulmonary embolism. In severe hypotension and respiratory collapse associated with massive pulmonary embolism, combined respiratory and metabolic acidosis (lactic acidosis) with hypercapnia can be seen.
Elevation of BNP and D-dimer can be attributed to pulmonary embolism and RV heart failure, and the increase in SGPT and SGOT is likely due to liver congestion. CT pulmonary angiography is the first choice for diagnostic imaging modality for pulmonary embolism; when contraindicated (e.g., pregnancy), a V/Q scan can be used instead. In the present case, chest CT confirms pulmonary embolism as it has demonstrated intraluminal filling defects in bilateral pulmonary arteries.
*Other causes of low voltage ECG include but are not limited to obesity, pericardial effusion, progressive cardiac myocarditis, or cardiomyopathy.
**Poor R wave progression in the chest leads can be seen in old anterior-septal MI,
cardiomyopathy, LVH, LBBB, and RVH/COPD (e.g., the present case).
***T wave inversion in the right precordial leads can be associated with anterior-septal ischemia or MI, myopericarditis, cardiomyopathy, and RV strain/ischemia (e.g., the present case).
Keywords:
chronic obstructive pulmonary disease, D-dimer, pulmonary embolism, P pulmonale
UpToDate:
Clinical presentation, evaluation, and diagnosis of the adult with suspected acutepulmonary embolism
Overview of acute pulmonary embolism in adults

Case 34 Content When this 78-year-old man walked into the clinic, he looked weary and depleted. For the past two days, he had been battling an intermittent fever topping 37.8°C, accompanied by a vanis
This 69-year-old man had been in good health until two days before admission when he returned from a beach. He experienced general weakness with chest tightness and shortness of breath (SOB) associated with watery diarrhea, nausea, and vomiting.
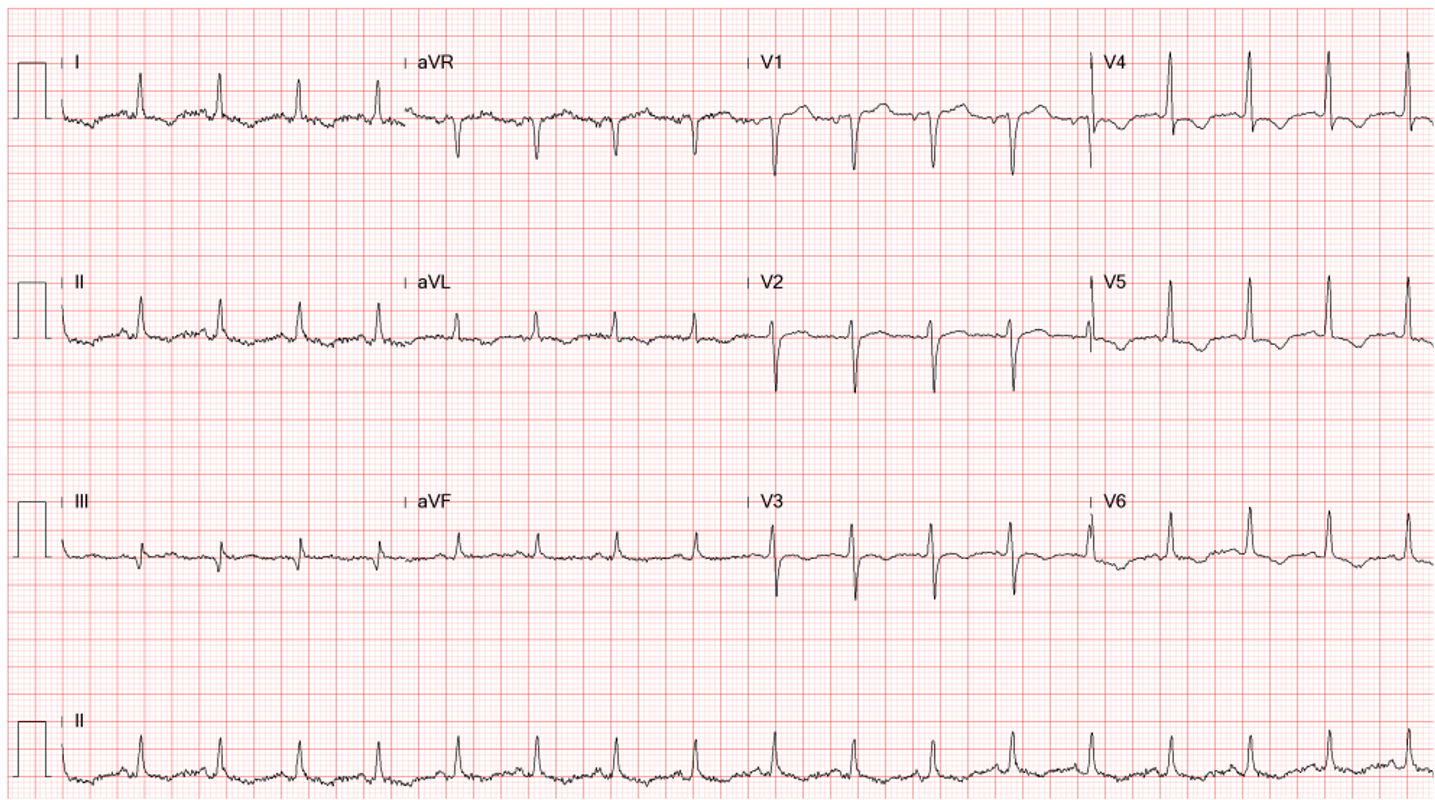
This 50-year-old man came to the Emergency Department complaining of having substernal chest pain for more than 10 hours. The pain was sharp and not exertion-related. It could radiate to the left shoulder, back, and scapula. It seemed positional, as inspiration could worsen it, and leaning forward could somewhat mitigate the pain. At times, he also experienced nausea, dyspnea, and cold sweats. Reportedly, he had flu-like symptoms with a runny nose and sore throat but didn’t visit any clinic seeking help. Past medical history was significant for thalassemia, mild GERD, and gallbladder stone diagnosed ten years ago.
If you have further questions or have interesting ECGs that you would like to share with us, please email me.
©Ruey J. Sung, All Rights Reserved. Designed By 青澄設計 Greencle Design.